Here are the poll results:
- Adenovirus (4%, 7 Votes)
- Herpes simplex virus (9%, 21 Votes)
- Human immunodeficiency virus (0%, 0 Votes)
- Human Papillomavirus (11%, 21 Votes)
- Mycoplasma genitalium (72%, 136 Votes)
- Unknown cause (4%, 8 Votes)
Most of our clever readers voted for the correct answer: Mycoplasma genitalium.
This case is closed. Thanks to everyone who voted. Read on to learn more about Mycoplasma genitalium.
What is Mycoplasma genitalium?
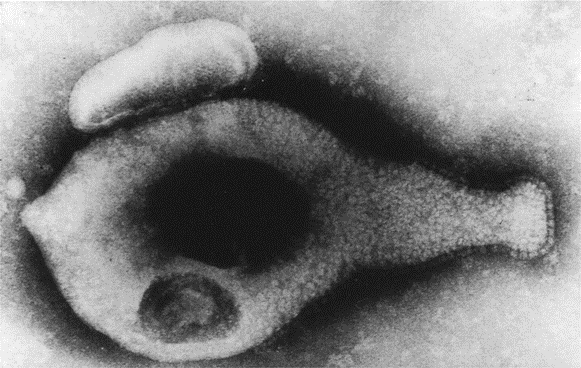
Mycoplasma genitalium (MG) is the smallest known bacterium that can replicate itself1. It typically invades the cells lining the genital and urinary tracts (epithelial cells), but has also been found in these cells in the rectum (end of the bowel) and lungs. Mycoplasma genitalium was first isolated from the human urogenital tract in the 1980s. The U.S. Centers for Disease Control and Prevention’s (CDC) most recent guidelines for sexually transmitted diseases (STDs)2 have highlighted M. genitalium as an emerging issue.
What are the symptoms?1
An MG infection often goes unnoticed, as most people have no symptoms.
Women can experience:
- Vaginal discharge
- Pelvic pain
- Bleeding after intercourse
- Bleeding between periods
In men, symptoms include:
- Pain on urinating
- Discharge from the urethra (tube through which urine passes out of the penis)
- Penile irritation and pain
What are the possible complications?
As most people are unaware of infection, the true complication rate is not known.
In women, infection has been associated with:
- Pelvic inflammatory disease, which in turn can damage the fallopian tubes and cause fertility problems
- Sexually associated reactive arthritis (arthritis triggered by infection)
- Premature birth
- Miscarriage
- Stillbirth
In men, infection has been associated with:
- Sexually associated reactive arthritis
- Pain and swelling of the testicles because of inflammation of the epididymitis (the tube that stores sperm)
How is it diagnosed?
Diagnostically, the only option is detection using a nucleic acid amplification test (NAAT). M. genitalium is a fastidious organism and can take up to six months to grow in culture.
How is it treated?
M. genitalium lacks a cell wall, and thus antibiotics targeting cell-wall biosynthesis (e.g., beta-lactams including penicillins and cephalosporins) are ineffective against this organism. Given the diagnostic challenges, treatment of most M. genitalium infections will occur in the context of syndromic management for urethritis, cervicitis, and PID.2
References:
- National Health Service 2018, United Kingdom, accessed 30 July 2019, <https://www.nhs.uk/news/medical-practice/new-guidelines-issued-sti-most-people-have-never-heard/>
- Workowski K, Bolan G. Sexually Transmitted Diseases Treatment Guidelines, 2015. MMWR Recomm Rep 2015;64(3):1-135.



0 Comments
Trackbacks/Pingbacks